Healthcare data doesn’t forgive mistakes. A misconfigured access control, an untested workflow, an unreviewed policy any one of these can turn into a HIPAA violation, a breach notification, and a fine that dwarfs whatever was saved by cutting corners on compliance. The organizations that stay compliant aren’t necessarily the ones with the biggest legal teams; they’re the ones that built the right combination of processes, people, and software solutions around their compliance work.
This guide covers the best HIPAA compliance software available in 2026, breaks down the core HIPAA principles every compliance team needs to understand, examines how AI is reshaping both the threat landscape and the compliance tooling, and explains why testing software like Testomat.io belongs in any serious healthcare organization’s compliance stack.
What HIPAA Compliance Requires
Before evaluating any HIPAA compliance platform, it helps to be clear on what HIPAA requires. The Health Insurance Portability and Accountability Act sets out a framework of rules designed to protect patient data, specifically, protected health information (PHI) — across healthcare providers, insurers, and their business associates. HIPAA compliance is structured around three core rules.
The Privacy Rule
The HIPAA Privacy Rule establishes standards for how covered entities and business associates can use and disclose PHI. It gives patients rights over their own health information, the right to access it, request corrections, and understand who has seen it. For compliance teams, this means having documented policies and procedures for every scenario where PHI could be accessed, shared, or used.
The Security Rule
The HIPAA Security Rule focuses specifically on electronic PHI (ePHI). It requires covered entities to implement three categories of safeguards:
- Administrative safeguards — risk analysis, workforce training, access management policies, contingency planning
- Physical safeguards — facility access controls, workstation security, device and media controls
- HIPAA technical safeguards — access controls, audit controls, integrity controls, transmission security
The Security Rule is where most technical compliance work happens, and where software tools have the most leverage.
The Breach Notification Rule
The Breach Notification Rule requires covered entities to notify affected individuals, the Department of Health and Human Services (HHS), and in some cases the media when a breach of unsecured PHI occurs. Timelines are strict: individual notifications within 60 days of discovery, HHS notification varies by breach size. Compliance teams need processes in place to detect breaches quickly and respond within those windows.
💡 Tip: HIPAA defines outcomes. That means your compliance program needs to document why your technical choices meet the requirements, not just that you made them. This documentation is exactly what auditors look at.
HIPAA’s Core Principles
Understanding the principles behind HIPAA helps compliance teams make better decisions when the rules are ambiguous, which is often.
- Minimum necessary. When using or disclosing PHI, you should access only the minimum amount necessary to accomplish the purpose. This principle runs through everything from access control configuration to how your development and QA teams handle test data.
- Reasonable and appropriate safeguards. HIPAA demands reasonable and appropriate security given your organization’s size, capabilities, and the nature of the PHI you handle. A 10-person clinic has different obligations than a major hospital network.
- Risk-based approach. All three sets of HIPAA safeguards are grounded in risk management. You can’t protect PHI without first understanding where it lives, who can access it, and what threatens it. HIPAA requires documented risk assessments and ongoing risk management, not a one-time checkbox exercise.
- Workforce accountability. HIPAA explicitly covers people, not just systems. Every employee who handles PHI needs training, clear policies, and accountability mechanisms. Many HIPAA violations trace back to workforce behavior rather than technical failures.
- Business associate management. Any vendor, contractor, or service provider that touches PHI on your behalf is a business associate and must sign a Business Associate Agreement (BAA) with appropriate HIPAA controls in place. Managing your business associate relationships is itself a compliance requirement.
How AI Is Changing HIPAA Compliance

AI is reshaping HIPAA compliance from two directions simultaneously, creating new risks while also providing new tools to manage them.
- AI systems often need access to real patient data. Training and fine-tuning AI models on clinical data raises immediate HIPAA questions: Is the data de-identified? Who has access to the training pipeline? Are your model outputs capable of re-identifying patients? These are questions most compliance frameworks weren’t built to answer, and most healthcare organizations are navigating them without settled guidance.
- AI-powered clinical tools create new PHI flows. When a healthcare provider uses an AI assistant to summarize patient records or suggest diagnoses, PHI is flowing through systems that may not be covered under existing BAAs. Every AI tool that touches patient data needs to be evaluated as a potential business associate.
- Generative AI introduces data leakage risks. Employees using general-purpose AI tools — ChatGPT, Copilot, and similar — for work tasks may inadvertently include PHI in their prompts. Without clear policies and technical controls, this creates a compliance exposure that’s genuinely hard to audit.
- AI testing requires careful data handling. AI model testing in healthcare contexts raises specific HIPAA concerns: if you’re testing an AI system against real clinical data, that testing process itself must comply with HIPAA’s technical safeguards. Using properly de-identified or synthetic test data isn’t optional — it’s a compliance requirement.
🤖 AI Model Testing: Methods, Challenges & Best Practices — Essential reading for teams testing AI systems that handle clinical or patient data under HIPAA.
How AI Helps With Compliance
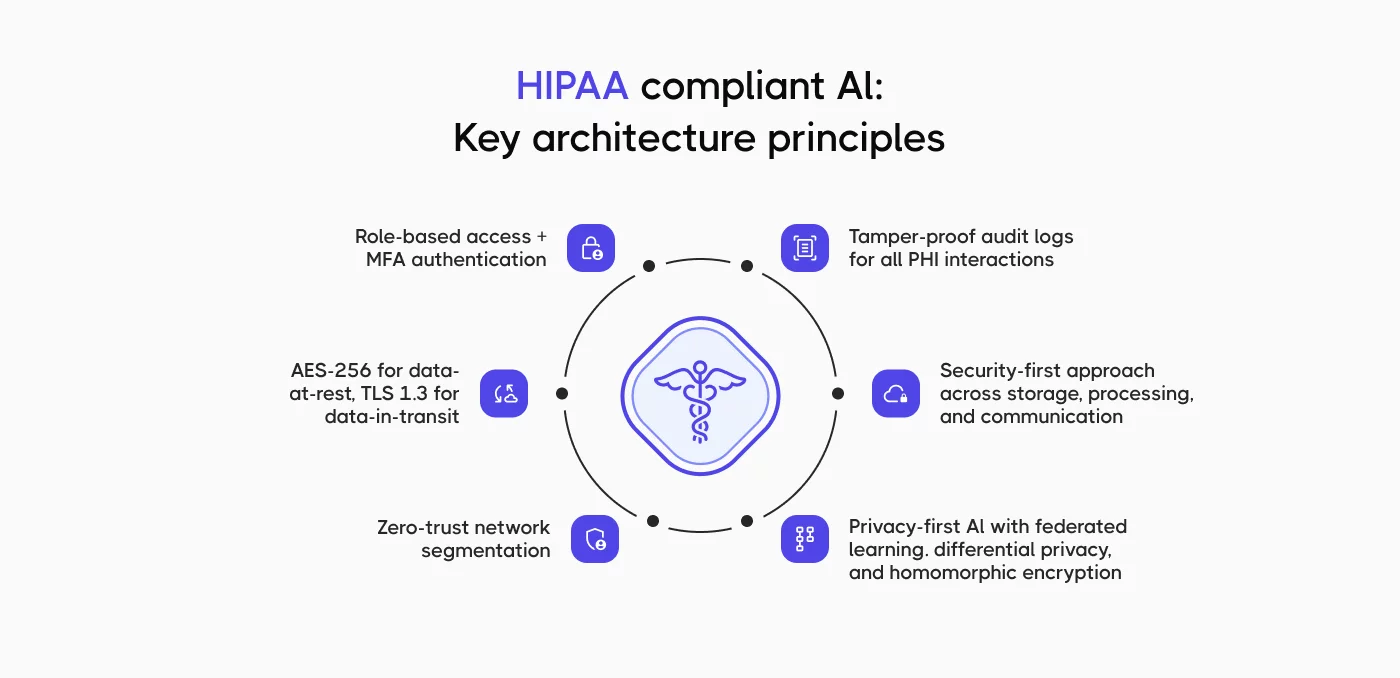
On the other side, AI is making compliance work meaningfully faster and more reliable:
- Automated evidence collection. Instead of manually gathering screenshots, logs, and audit trails, AI-powered compliance platforms can continuously monitor systems and collect evidence automatically, reducing manual effort by up to 70-80% on evidence-intensive tasks.
- Continuous control monitoring. AI enables compliance platforms to monitor security controls 24/7, flagging misconfigurations or access control drift the moment it occurs rather than at the next scheduled audit.
- Intelligent risk assessment. AI can analyze large volumes of system data to surface risk patterns that human reviewers would miss, identifying, for example, that a specific combination of access privileges creates elevated PHI exposure risk.
- Policy gap analysis. AI tools can compare your current policy library against updated regulatory requirements and flag gaps, reducing the risk that a policy update gets missed.
💡 Tip: When evaluating AI-powered compliance tools, ask specifically how they handle the data they ingest. A compliance platform that processes your PHI to do its job is itself a business associate and needs a BAA, the same rules apply.
Why Software Testing Is a HIPAA Compliance Requirement
This point gets skipped in most HIPAA compliance software roundups, but it’s worth stating clearly: your software testing process is part of your HIPAA compliance program, not separate from it.
The HIPAA Security Rule’s technical safeguards require that ePHI systems are protected against unauthorized access, that integrity is maintained, and that transmission is secure. Meeting those requirements isn’t just about configuration — it requires systematic testing to verify that the controls actually work.
- Audit controls (§ 164.312(b)) require mechanisms to examine activity in systems containing PHI. Testing those audit mechanisms — verifying that logs capture the right events, that alerts fire correctly, that access controls block unauthorized users — is how you know they work.
- Access controls (§ 164.312(a)(1)) require technical policies to allow only authorized persons to access ePHI. Role-based access control is only as good as the test coverage that validates it. If you haven’t tested that users with a given role can’t access PHI they shouldn’t see, you don’t know that your access control is working.
- Integrity controls (§ 164.312(c)(1)) require mechanisms to ensure ePHI isn’t improperly altered or destroyed. This is a direct mandate for automated testing of data integrity in any system that stores or transmits PHI.
This is where Testomat.io becomes relevant to HIPAA compliance — not as a compliance automation platform per se, but as the testing infrastructure that validates your technical safeguards actually do what they’re supposed to do.
How Testomat.io Supports HIPAA-Compliant Software Testing
Testomat.io is a modern AI-powered test management platform that helps QA teams organize, execute, and track both manual and automated tests across any environment. For healthcare organizations building or maintaining ePHI systems, it provides several capabilities that directly support HIPAA compliance:
- Traceability from requirement to test to result. HIPAA auditors want to see that your technical safeguards are working. Testomat.io’s traceability matrix links compliance requirements to specific test cases and to test execution results, so when an auditor asks how you know your access controls work, you have a documented, timestamped answer.
- Audit-ready test reports. Testomat.io generates detailed test reports that capture what was tested, when, by whom, and what the result was. These reports are exactly the kind of documentation that demonstrates ongoing compliance monitoring, which HIPAA requires.
- Continuous test execution via CI/CD. HIPAA’s Security Rule isn’t a one-time checkbox — it requires ongoing safeguards. Testomat.io integrates with GitHub Actions, GitLab, Jenkins, and Azure DevOps to run tests automatically on every code change, ensuring that security controls are continuously validated rather than reviewed once a year before an audit.
- Role-based access controls and audit logs. Testomat.io’s own platform supports role-based access and maintains an audit log of changes, important when the platform itself is handling sensitive test documentation related to PHI systems.
- AI test generation for compliance test coverage. The Enterprise tier includes AI-powered test generation that can help teams build out test coverage for compliance-sensitive scenarios faster, particularly useful when documenting coverage across HIPAA’s specific technical safeguard requirements.
For healthcare engineering teams that take their compliance obligations seriously, having a well-organized test management system is part of demonstrating that your security controls are continuously validated.
📋 11 Best AI Test Management Tools 2026 — A broader look at AI-powered test management platforms and how they support quality in regulated industries.
Best HIPAA Compliance Software Platforms in 2026
With the technical and regulatory context established, here’s a detailed look at the leading HIPAA compliance platforms.
Sprinto
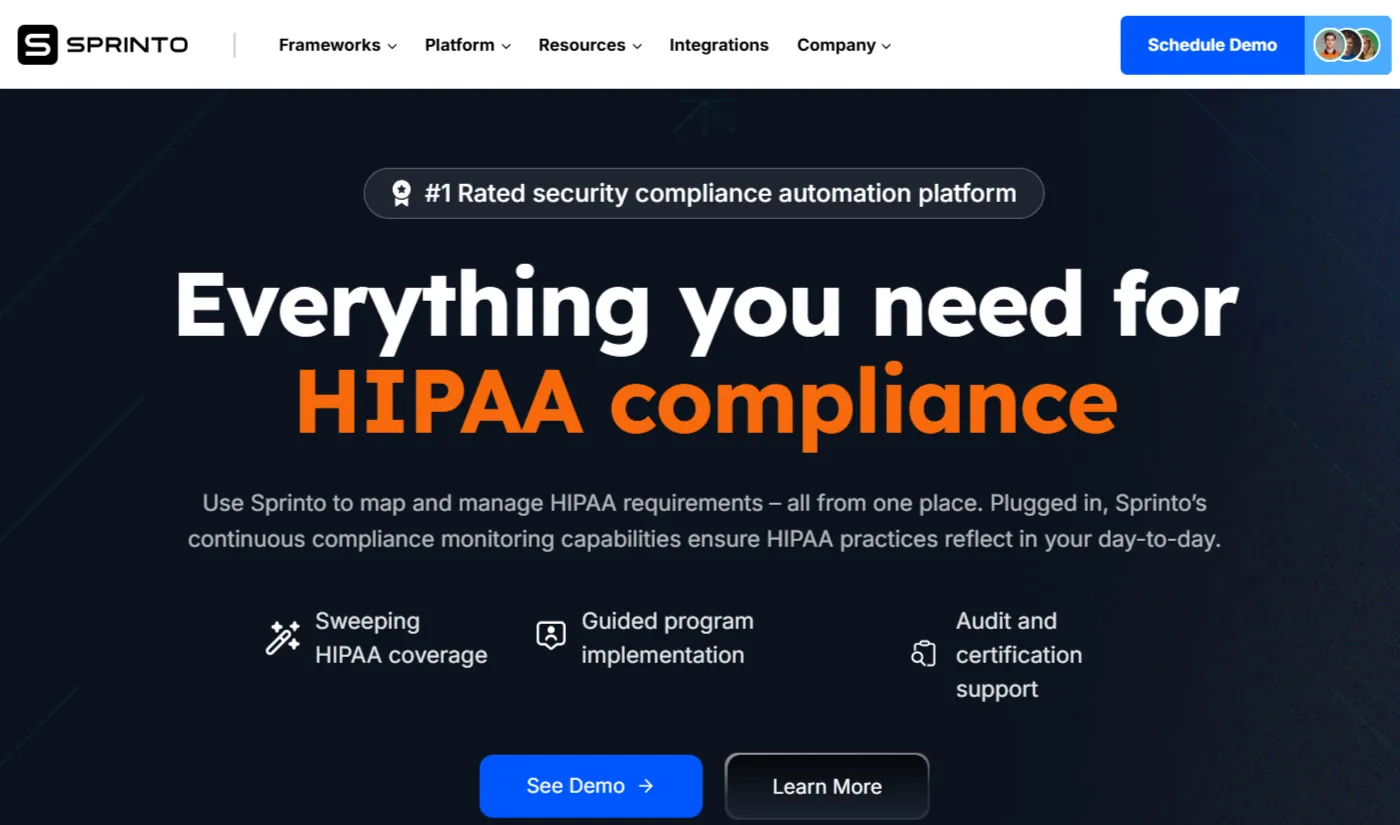
Sprinto is a solid HIPAA compliance software choice for healthcare companies that need continuous monitoring and automated evidence collection without significant customization. Its strength is simplifying audit preparation, it automates security measures, gathers evidence, and provides separate dashboards for internal and external auditors that show criteria, controls, and asset statuses at a glance.
Key features:
- Policy management dashboard for creating, sharing, and tracking HIPAA-compliant policies across the organization
- Automated evidence collection from AWS, GCP, and Azure
- Audit support with pre-configured reports aligned to HIPAA standards and dedicated auditor views
Hyperproof
Hyperproof positions itself around workflow management and evidence organization. For compliance teams that spend a lot of time coordinating between tools and people, its integrations with Slack, Microsoft Teams, Google Drive, and SharePoint are genuinely useful, they bring compliance tasks into the systems where work actually happens rather than requiring everyone to live in yet another dedicated platform.
Key features:
- HIPAA program template with recommended security actions and controls
- Automated evidence collection integrated directly with requirements and controls
- Integrations with collaboration tools for streamlined workflows
Drata

Drata is a well-established compliance automation platform with multi-framework support and strong employee training capabilities. For organizations that need to maintain HIPAA compliance alongside SOC 2, ISO 27001, or other frameworks, Drata’s ability to handle multiple compliance programs from one platform reduces the overhead of running parallel compliance efforts.
Its integration with tools like AWS, Okta, and GitHub means evidence collection can be largely automated from existing infrastructure — the platform pulls data from the systems you already use rather than requiring manual exports.
Key features:
- Integrations with AWS, Okta, GitHub, and other tools for automated data collection and verification
- Built-in HIPAA security training and compliance awareness tracking for employees
- Audit-ready reports summarizing compliance efforts, including evidence of controls, policies, and risk assessments
Secureframe
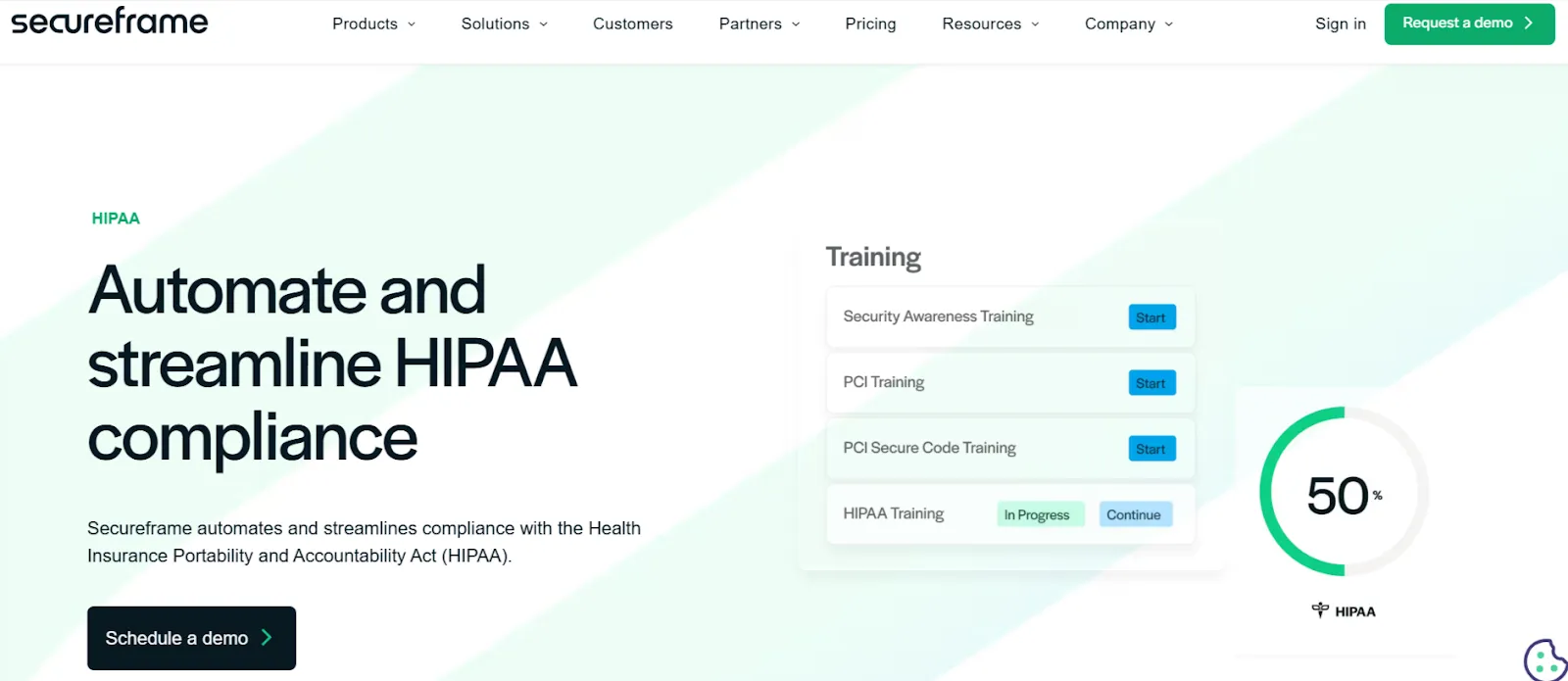
Secureframe takes a user-experience-first approach to HIPAA compliance. Its interface is among the cleaner ones in this category, and the self-serve employee training flow — where staff are guided through HIPAA privacy and security training including quizzes and policy acceptance — is particularly well-executed. For organizations where getting staff through compliance training is a perennial challenge, Secureframe makes that easier.
Key features:
- HIPAA policy creation with a library of adaptable policies publishable directly to employees via the platform
- Employee training with progress dashboard, quizzes, and automated, self-serve training flow
- Centralized documentation and evidence repository, with automatic evidence collection from integrated security systems
Choosing the Right HIPAA Compliance Tool
No single platform is the right HIPAA compliance software for every organization. The right choice depends on several practical factors:
- Your compliance scope. If HIPAA is your only compliance requirement, a simpler platform may serve you well. If you also need to maintain HIPAA alongside SOC 2, ISO 27001, or GDPR, choose a platform with genuine multi-framework support rather than bolted-on coverage.
- Your team’s technical depth. Some platforms assume significant compliance expertise and reward it. Others are built for teams that need more guidance. Be honest about where your team is.
- Your evidence collection needs. If most of your PHI systems live in AWS, GCP, or Azure, the quality of a platform’s cloud integrations matters enormously. A platform with shallow integrations will leave you filling gaps manually.
- The role of human expertise. Scrut’s access to in-house HIPAA auditors and consultants is a meaningful differentiator if your team hasn’t been through a HIPAA audit before. Software doesn’t replace the judgment that experienced compliance professionals bring to ambiguous situations.
- Your software testing posture. If your organization builds or maintains software that handles ePHI, your test management system is part of your compliance program. Testomat.io’s traceability matrix, automated test reporting, and CI/CD integration make it a natural complement to any HIPAA compliance platform, providing the technical evidence layer that demonstrates your security controls are continuously validated.
💡 Tip: When evaluating HIPAA compliance software, ask vendors directly: “What does your audit trail look like, and can I export it in a format my auditor can work with?” The answer tells you a lot about how seriously the platform takes the actual audit experience rather than just day-to-day compliance tracking.
Building software that handles patient data? Testomat.io helps healthcare engineering and QA teams maintain continuous test coverage with full traceability, so your technical safeguards are always documented, validated, and audit-ready.
Frequently asked questions
What is HIPAA compliance software and what does it do?

HIPAA compliance software is a platform designed to help covered entities and business associates implement, monitor, and document the administrative, physical, and technical safeguards required by the HIPAA Security Rule — and the policies and procedures required by the Privacy Rule. In practice, these tools automate evidence collection, continuously monitor security controls, manage policy libraries, track employee training completion, support risk assessments, and generate documentation for audits. The best platforms reduce the manual effort required to achieve and maintain HIPAA compliance significantly — some by up to 70-80% on evidence-heavy tasks.
Does HIPAA compliance software replace the need for a compliance expert?

No. HIPAA compliance software automates repeatable tasks — evidence collection, control monitoring, policy distribution — but it doesn’t replace the judgment that experienced compliance professionals bring to ambiguous situations, vendor contract negotiations, breach response, and audit preparation. The strongest platforms, like Scrut Automation, recognize this and combine automation with access to in-house HIPAA auditors and consultants. Software handles the volume; experts handle the judgment calls.
Is software testing required for HIPAA compliance?

Yes, in practice — though HIPAA frames it in terms of outcomes rather than mandating specific testing practices. The Security Rule’s technical safeguards (access controls, audit controls, integrity controls, transmission security) all require organizations to demonstrate that their ePHI systems function as intended. The only reliable way to demonstrate that is through documented, systematic testing. Healthcare engineering teams that use a test management platform like Testomat.io can link specific test cases to HIPAA control requirements, maintain timestamped execution records, and generate audit-ready reports — exactly the kind of evidence that satisfies auditors and supports ongoing compliance monitoring.
How often do HIPAA risk assessments need to be performed?

HIPAA requires a risk analysis to be conducted initially and then reviewed and updated periodically — but it doesn’t define “periodically” as a specific interval. The practical answer is: whenever your environment changes significantly (new systems, new services, changes in how PHI is handled), and at a minimum annually as part of your ongoing compliance program. Most compliance platforms, including Scrut and Drata, support continuous monitoring that effectively turns risk assessment from a periodic event into an ongoing process.